Taking Blood Pressure
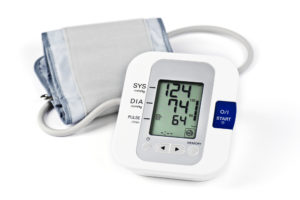 We’re all used to seeing people having their blood pressure (BP) taken in the arm, but if you need to keep track of it for your GP or treatment programme, and have short or deficient arms, you’ll need to take it in the leg.
We’re all used to seeing people having their blood pressure (BP) taken in the arm, but if you need to keep track of it for your GP or treatment programme, and have short or deficient arms, you’ll need to take it in the leg.
There is currently no, approved, blood pressure device for the leg so it’s best to use a conventional blood pressure cuff. Leg BP is different to arm BP, but will still indicate whether your BP is normal or raised. Your doctor will be able to interpret the readings for you.
Here's our simple guide to taking your blood pressure this way.
You can also watch a webinar presented by Dr Susan Brennan on the importance of getting your blood pressure checked to monitor your health and help prevent serious illness.
Blood pressure webinar and video
Watch our video demonstrating how to take blood pressure correctly using a cuff around the leg.
Dr Susan Brennan presents a webinar on the importance of monitoring your blood pressure
Taking blood pressure in the leg
1. Measure blood pressure in the same way, using a monitor, and with the same sized cuff, as your doctor so you can compare results
You can buy blood pressure monitors in pharmacies and online, but be sure to buy a clinically validated monitor and the correct cuff size for the area it is to be used on.
Read the BIHS guide to using automated blood pressure monitors
Cuff sizes are 'large' for a thigh (circumference of less than 50cm) and 'standard' (circumference less than 33 cm) or 'small' (less than 23cm) for a calf or ankle. If you’re not sure which size is best, contact the company supplying your blood pressure device.
2. Always measure your blood pressure at the same site (thigh, calf or ankle) and at the same time of day.
Take your blood pressure at least once a day – but preferably twice – for 7 days before you visit your GP. Keep a record of the readings.
Lots of things can raise your blood pressure briefly so, before you take it, make sure you don’t need the loo, that you haven’t just eaten a big meal and that it’s more than 30 minutes since you’ve drunk anything caffeinated or smoked a cigarette.
3. Wear loose-fitting clothes.
4. Take your blood pressure carefully and consistently following these steps:
Put the blood pressure cuff around your thigh, calf or ankle on the part that is correct for the cuff. It doesn’t matter which leg you use but continue to use the same one; using the ankle may be less painful than the calf.
Make sure your leg is slightly raised by placing it on a pillow or cushion so that the cuff is at about the same level as your heart.
Lie back and relax for ten minutes with your head on a pillow before switching on your automatic blood pressure monitor.
Keep still and silent when you’re taking your reading; moving and talking can mess it up.
Take three readings about two minutes apart.
Record your readings in the memory of your monitor, on a computer or on paper. If in doubt, talk to your doctor.
5. Take a look at these common concerns.
BP medication
Some people affected by thalidomide are worried that drugs affect them more than other people. This isn’t normally the case; but if you’re concerned how medicine to lower your BP may affect you, have a chat with your doctor.
You might agree to start off at a lower dose, which is much better than not taking it at all.
Difficulty having blood taken
If it’s not easy for professionals to take samples of your blood, it may make it more difficult to assess your risk of heart attack or stroke or how well drugs you’re taking are working.
Certain medications don’t need to be monitored by regular blood tests so ask your doctor if they can prescribe those.
Want to know more?
Call the Thalidomide Trust's Health and Wellbeing team on 01480 474074. We're happy to help.
Download this information as a factsheet
Taking Blood Pressure
Take a look at the information from the recent Blood Pressure Awareness week
