The Pain And Self-Care Cycles
Left untreated pain can persist, affecting lives both physically and mentally in a repeated cycle.
To help break this cycle there are a number of things you can do to help yourself.
What is the pain cycle?
The pain cycle, illustrated below, shows how persistent pain can result in lack of movement, low mood, negative thinking which then worsens the persistent pain, and the cycle continues, adversely affecting all areas of your life.
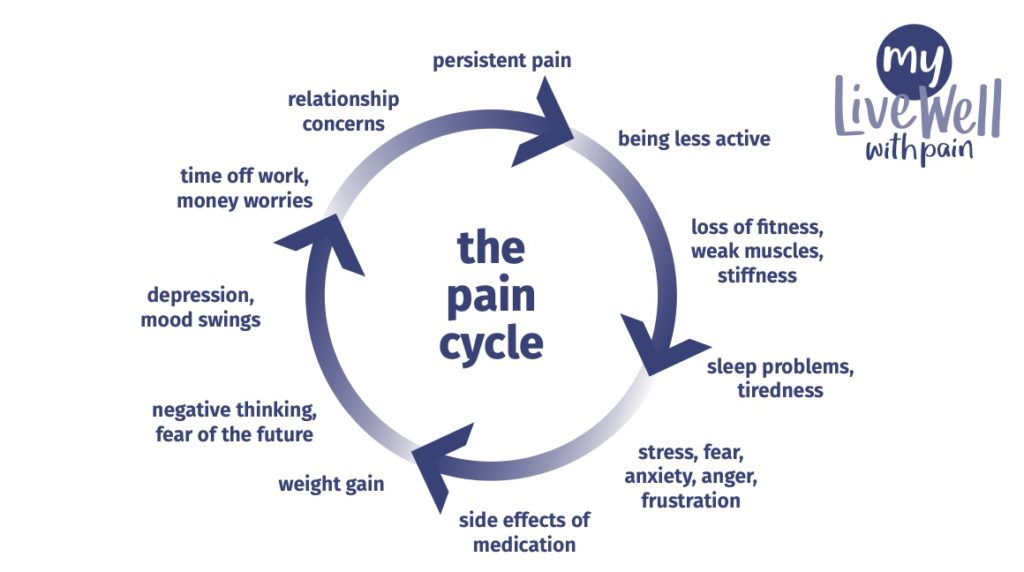
To improve pain, we must break the cycle.
What breaks the pain cycle? The self-care cycle!
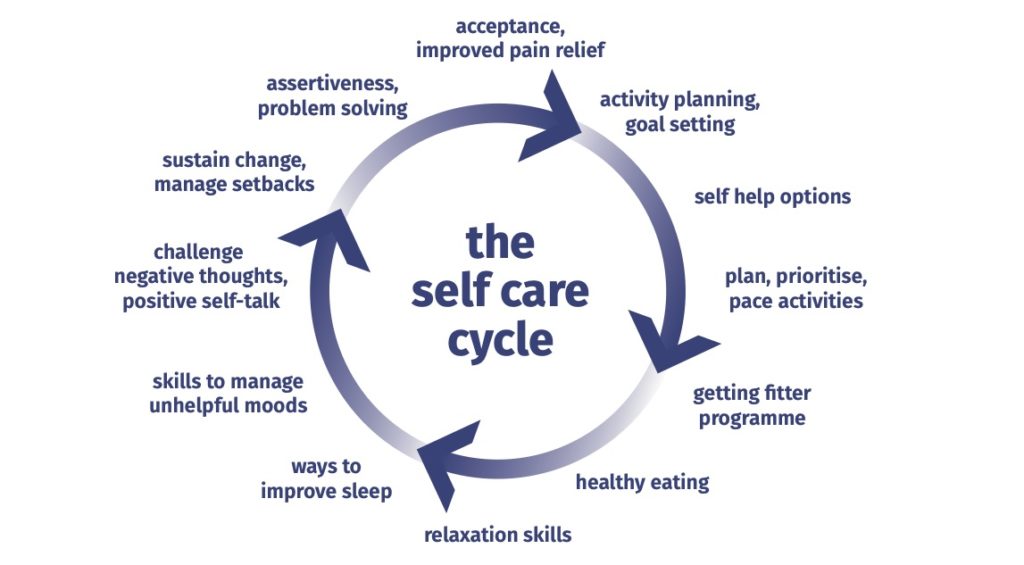
The self-management skills page on the Live Well With Pain website shows all the things you can do to help break the pain cycle. Self-care simply means all the things you can do to care for yourself.
This can be focussing on planning your activities, getting fitter and eating healthily, managing your moods to address negative thoughts and sustain positive changes leading to a cycle of positive actions.
What is Pacing?
Pacing refers to breaking down a particular task into chunks of time and having regular breaks before the pain comes on. It may mean you can do more over time and breaks the so-called boom and bust cycle, where on a good day you do a lot and then you are wiped out with pain and fatigue for a few days.
In addition….
Remember that with short arms you have to rely on muscles in the neck and back to support your arms constantly. Find other ways to support your arms periodically, say for a short time every 15 minutes, to give your neck and shoulders a rest: –
- Rest your arms on a cushion.
- Occasionally sit sideways to rest the arm on the back of the chair.
- If standing for long periods lean each arm on a surface.
Delegating tasks
If it is possible, can you delegate less enjoyable and more onerous tasks to others to preserve yourself for the things you really enjoy? Or consider using your health grant to pay someone to do these tasks for you? For example, if housework really puts strain on your arms and shoulders, consider getting a cleaner and instead preserve the function in your joints for activities you get real enjoyment out of, like painting or gardening.
Consider gadgets to help everyday life to reduce the amount of strain on your body. There is a balance between the idea of “use it or lose it” as compared with protecting your body and joints so they wear out less quickly.
To find out more about gadgets that can help you can phone the Health & Wellbeing team on 01480 474074 for help and advice.
Meditation and relaxation skills
Some people find meditation a useful way to help cope with chronic pain and some pain clinics also recommend it too.
Some people also find apps like Headspace or Calm helpful. These are forms of mindfulness which is a type of meditation that simply means being present and focusing on the moment, rather than thinking about the past or the future.
What meditation can I try?
Guided pain management meditation – from Meditainment
Mindfulness based pain management meditations – from the Pain Management Centre, University College Hospital London on the Soundcloud website
Many activities can be done mindfully as well - these include gardening, painting, tai chi and even doing a crossword.
Movement or exercise
Being more active can help in many ways. Movement can help loosen tight muscles, help build muscle to support our joints, but also helps us feel better by releasing feel good hormones and reduce anxiety, all of which can help us live well with pain.
It can be absolutely anything, but the key thing is it has to be something you enjoy. It can include walking, Pilates, chair-based yoga, gardening, swimming or even singing can help.
If you haven’t exercised in a while or are worried about how to exercise safely, getting an assessment from a physiotherapist can be an excellent place to start. This is also important if you have short arms as you may be unintentionally causing further wear and tear on your shoulder muscles by exercising the damaged muscles instead of exercising the supportive muscles, so getting some advice is key.
Find a local physiotherapist on the Chartered Society of Physiotherapy website or ask the Health and Wellbeing team at the Trust, 01480 474074 or email.
How can physiotherapy help?
Take a look at this video showing how physiotherapy for thalidomide survivors, combined with targeted exercise, can help reduce pain.
Healthy eating and nutrition
You are what you are eat! I’m sure you’ve heard this before. There are lots of links between what we eat and the way we feel. Having a good diet can help weight management and help reduce the strain on joints. What we eat and our weight also has an impact on other conditions like blood pressure, heart disease and diabetes.
What we eat can help the function of the nervous system, our immune and hormone systems which can direct the way we experience pain.
The diet with the best evidence for improving our health is the Mediterranean diet. This is a diet based on natural, unprocessed foods such as vegetables, fruit, nuts, olive oil, fish and wholegrains.
To find out more about losing weight to improve your health see Dr. Chatterjee’s ‘Feel Great Lose Weight’ to find an approach to a lasting and sustainable weight loss solution that works for you.
Sleep
When you’re in pain, you often sleep badly or have an interrupted night’s sleep. This in turn often makes your pain worse and you can find it even harder to sleep, and so the cycle continues.
There are a few simple things you can do to help get a better night sleep:
- Switch off mobiles and tablets 90 minutes before bed.
- Keep your bedroom cool, dark and tidy.
- Stick to a routine and try and go to bed and get up at the same time each night.
- Try and get some natural light as soon as you get up, either by going outside or sitting by a window.
- Try some gentle exercise such as yoga, Pilates or a walk.
- Keep your bedroom just for sleeping and sex – don’t work or watch TV in your room.
Also
Think about how well supported you are in bed. If your arms are not long enough to reach the pillow, use extra pillows to support them.
Here are some more tips on improving sleep from the charity, Mind.
If the tips from Mind aren’t helping, consider asking your GP to refer you for Cognitive Behavioural Therapy (CBT). This can be very helpful for insomnia.
You could also try an online 6-week programme called Sleepio. This is free on the NHS in some areas, otherwise you may have to pay a fee which is around £3.95 a week.
Managing Mood
Pain can worsen our mood and cause anxiety or depression. Equally when we are depressed or anxious, this can make our pain more intense and for longer periods. Treating anxiety and depression is really important if we want to improve the pain we experience.
Mind suggests the following things that you may find helpful;
- Talk to someone you trust. If you aren't able to open up to someone close to you, the Samaritans run a 24-hour helpline that you can call to talk to someone confidentially.
- Try Mindfulness (see above).
- Spend time in nature and green spaces.
- Try and exercise or move daily e.g. yoga, Pilates, gardening.
- Keep a mood diary.
- Practice self-care which means doing the things that you enjoy e.g. listening to music, having a massage, doing a crossword.
- Peer support brings together people who've had similar experiences to support each other.
The importance of connecting with others

Many people find it helps them to share ideas about how to stay well, connect with others and feel less alone. You could:
- Contact a specialist organisation. For example, you can find details of support groups, forums and helplines on the SANE and CALM websites.
- Join Side By Side (formerly Elefriends), Mind's supportive online community.
- Contact Mind's Infoline 0300 123 3393 and ask about support groups near you.
- Contact the Trust to be put in touch with a trained volunteer as part of our Talk Together service.
- Join the Trust's meet up group, Positively Connected, to connect with other beneficiaries through shared interests and coffee morning chats.
How can I get help with low mood and depression?
The Trust run a programme, called “Lift-Up”. Lift-Up is a self-help service to support those who are experiencing low mood.
It includes support by a trained beneficiary Lift-Up supporter with a weekly telephone call to help you understand what low mood is and how to make changes to improve your mood.
The NHS have a self-help guide for depression that uses cognitive behavioural therapy.
Remember that you can seek professional help for depression, anxiety or stress if you are feeling overwhelmed – do speak to your GP.