Sleep Awareness Week
 Welcome to Sleep Awareness Week. We are making this awareness week all about sleep because many of you report experiencing sleep disturbance when we speak to you at HNA’s. Disturbances noted include having difficulty getting to sleep in the first place, waking frequently or waking early. The quality and quantity of our night’s sleep can have an effect on our general wellbeing, either on a specific day or over a longer period.
Welcome to Sleep Awareness Week. We are making this awareness week all about sleep because many of you report experiencing sleep disturbance when we speak to you at HNA’s. Disturbances noted include having difficulty getting to sleep in the first place, waking frequently or waking early. The quality and quantity of our night’s sleep can have an effect on our general wellbeing, either on a specific day or over a longer period.
Read on to find out what you can do yourself that can influence how well you sleep.
What can you do to give yourself the best opportunity of a good night’s sleep?
Lifestyle changes
If you are having trouble sleeping it is a good idea to take a look your lifestyle and evaluate if any small tweaks might help you have a more restful night that sees you feeling more refreshed the next day.
 We’ve all been told that caffeine can disrupt sleep. Try not to drink caffeine after midday to help you get a more restful night. Sugary drinks are also reported to cause difficulties with sleeping and worth thinking about cutting down on. Drinking alcohol can make you fall asleep faster but you are likely to be more wakeful and your night disrupted.
We’ve all been told that caffeine can disrupt sleep. Try not to drink caffeine after midday to help you get a more restful night. Sugary drinks are also reported to cause difficulties with sleeping and worth thinking about cutting down on. Drinking alcohol can make you fall asleep faster but you are likely to be more wakeful and your night disrupted.
 Smoking can have a side effect of sleep disruption as nicotine is such a potent stimulant. Reducing or stopping smoking can help you get a better night’s sleep.
Smoking can have a side effect of sleep disruption as nicotine is such a potent stimulant. Reducing or stopping smoking can help you get a better night’s sleep.
 Exercise can contribute to better sleep through altering the body’s hormonal profile in addition to reducing core body temperature. The form of exercise isn’t as important as simply doing some, so pick something you enjoy! However it is important not to exercise too close to bedtime as this can keep you awake.
Exercise can contribute to better sleep through altering the body’s hormonal profile in addition to reducing core body temperature. The form of exercise isn’t as important as simply doing some, so pick something you enjoy! However it is important not to exercise too close to bedtime as this can keep you awake.
Making a few changes in these areas could help to improve the sleep you get. There is not one formula that works for everyone, so experiment with what works for you and change things about if something is not working.
Other things that can help could include:
- Planning the following day’s tasks so that you do not have thoughts about this whizzing around in your head overnight
- Reconsider your use of electronic equipment before bed, ideally turning off our phone 90 minutes before you are heading to bed. Blue light emitted from your phone, tablet or the television has been shown to have an adverse effect on sleep. It is possible to buy a blue screen shield from Amazon that will reduce your exposure level before bed. Or alternatively could you listen to some relaxing music, an audio book or read instead?
- Incorporate relaxation techniques into your bedtime routine
- The use of some scents can enhance sleep, try lavender, ylang ylang and chamomile amongst others can induce a relaxing effect.
You can find more useful tips about sleep strategies on the Sleep Station website
Setting up your bedroom for the best night’s sleep
If possible keep your bedroom specifically for sleeping in. If you regularly use your bedroom as a games room, cinema or an office this can be a disruptive influence on your sleep. Your bedroom needs to be your retreat from everyday life, somewhere you can relax, and feel safe, away from the stresses of everyday life.
The temperature of your room can influence how well you sleep. The ideal temperature is between 16-18C but you’ll know yourself when you are too hot or too cold and when you have your optimum sleep. If not be mindful of this and adjust accordingly.
The amount of light in your bedroom can affect how well you sleep, if at night you can see the opposite wall of your room then your room is too bright.
Try to make sure your room is as quiet as possible so you won’t be disturbed.
Invest time and money in making the best bed choice. In your lifetime, you’ll spend more time in bed than you’ll spend in any other single location. In fact, by the time you are 70 you’ll have spent 25 years in bed. It’s undoubtedly crucial that you have the right bed for you. It is recommended that you invest in a new mattress once every eight years – is it time for you to pick a new one?
Naturally, creating the perfect bedroom environment is just a starting point for a good night’s sleep. Making sure all of these areas are as good as they can be in your set up.
Persistent Pain and Sleep
Many beneficiaries find it hard to get to sleep due to persistent pain, reporting that they wake frequently during the night, very early in the morning or feel unrefreshed or tired after their night’s sleep. In fact pain is the main cause of insomnia in the UK population.
There are a number of things you can try to set you up for a better night’s sleep when you suffer from persistent pain.
We would appreciate hearing about your experiences or any tips that you think may help others.
Please get in touch with our Health & Wellbeing team on 01480 474074 or by email to share your information.
Tips to Help Promote Sleep if You're Living With Persistent Pain
1. Consume foods that may help promote sleep
By including certain foods in your evening meal it may help increase the level of tryptophan in your body. Tryptophan is a type of protein that is essential for the production of the sleep-regulating hormone, serotonin. Increased tryptophan levels help reduce the time taken to fall asleep, promote more restful sleep, and improve alertness in the morning. Examples of such sleep-promoting foods are:
- Carbohydrates with a high glycemic index, such as rice.
- Fruits, such as cherries and kiwis.
- Whole foods, such as milk, pulses, fatty fish, and shellfish.
When you plan to make dietary changes, consult with your doctor to ensure that the new food or supplement that you try does not adversely affect any existing medical condition or medication that you may be taking.
2. Practice yoga daily
Yoga is a mind-body therapy and through the physical poses, rhythmic breathing, and meditation, yoga may help relieve persistent pain and improve sleep. It is advised to learn yoga from a licensed instructor who will be able to advise how to adapt the exercises for you if need be and who can tailor the poses according to your tolerance level. Once you learn the specific yogic poses, you can practice them at home at your convenience. If you experience pain or discomfort while doing a pose, make sure to inform your yoga instructor.
3. Take slow, deep breaths to get to sleep and fall back asleep
Slow, rhythmic breathing has calming mind-body effects and may help alleviate pain and stress, promoting sleep. Research indicates that taking slow and deep breaths before bedtime can help you get to sleep faster and fall back asleep in case you wake up during the night. This type of breathing technique also helps synchronize your heart rate and breathing pattern, which may help promote deeper, restorative sleep.
4. Consider taking a sleep aid
Several sleep-enhancing preparations are available over the counter to help promote better sleep. While some are available as tea bags for brewing, others can be taken orally in the form of tablets or capsules. Here are a few common examples:
- Herbal preparations: Valerian capsules and chamomile tea
- Fruit extracts: Cherry juice or capsules of tart cherry extract
- Micronutrient supplements: Zinc and/or magnesium
These supplements may help improve the onset, duration, and quality of sleep in some people.
When you are sleep deprived due to your persistent pain, it may be worth trying one or more of these little-known options to help you get more sleep. A process of trial and error will help you understand which option works best. If you’re not able to sleep well despite trying these tips, consult your GP or one of the Trust’s Medical Advisers for more advice.
Effects of Sleep Disruption Due to Persistent Pain
Research has demonstrated that disrupted sleep will, in turn, exacerbate persistent pain. A lack of restorative sleep also hampers the body’s immune response and can affect cognitive function. Thus, a vicious cycle develops in which the pain disrupts sleep, and difficulty sleeping makes the pain worse, which in turn makes sleeping more difficult, etc.
For people with persistent pain, trouble falling asleep is one of the most prevalent types of sleep disruption, however waking up during the night and waking earlier than desired are also frequent problems. In addition, many people with persistent pain do not feel refreshed in the morning when they awaken, a sleeping problem termed “non-restorative sleep.”
Trouble Falling Asleep
Persistent pain can impact sleep in a number of ways. To understand how a pain problem can make it difficult to fall asleep, it is helpful to think about the process associated with going to sleep for the night.
In getting ready for bed, it is common to eliminate all distractions or other influences in an effort to relax and fall asleep. This may include quieting the room, turning off the lights, eliminating any other noises, trying to get comfortable, and beginning to try to fall asleep.
However, this quieting of one's environment can cause problems for someone experiencing persistent pain, since the only thing left for the brain to focus on is the pain. People will often report that one of their primary pain management tools during the day is to distract themselves from their persistent pain by staying busy with other tasks (such as reading, watching television, engaging in hobbies or crafts, working, interacting with others, etc.).
When trying to fall asleep, there are no distractions except for the pain, and the perception of pain can actually increase. The longer falling asleep is delayed, the more stressful the situation becomes.
Problems Staying Asleep
Many people experiencing persistent pain also report awakening frequently during the night. These "microarousals" (a change in sleep state to a lighter stage of sleep) per hour of sleep, lead to awakenings and can be a significant intrusion into a night's sleep and disruptive to the normal stages of sleep.
This problem is often the cause of non-restorative sleep. Individuals with persistent pain often experience less deep sleep, more awakenings during the night, as well as less efficient sleep. Thus, the quality of sleep is often light and unrefreshing.
This non-restorative sleep pattern can then cause diminished energy, depressed mood, fatigue, and worse pain during the day.
Combatting Insomnia Caused by Persistent Pain
When addressing insomnia associated with persistent pain, it is important that the patient receives the best possible treatment for pain using a multidisciplinary approach.
Develop a Healthy Sleep/Wake Cycle
Keep a consistent bedtime/waking routine. Going to bed at the same time each night and getting up the same time in the morning — seven days a week — helps the body develop a healthy sleep-wake cycle. This is important even if you had difficulty falling asleep or awakened through the night. When you get up, exposing yourself to morning light by going outside or sitting by a bright window can help your body clock. One of the most common disrupted sleep-wake patterns for those with persistent pain is to "get sleep when I can." In this situation, an individual who did not fall sleep until 2 a.m. might compensate by "sleeping in" until noon. If this counterproductive pattern gets established, the routine sleep-wake cycle becomes more and more disrupted.
Avoid naps during the day. Although this may seem like a good idea if you experience a night of non-restorative sleep, it can actually make the situation worse over the long term.
Maintain a regular schedule. Despite your persistent pain try to eat your meals at the same time every day, engaging in other activities at regular times, such as a walk outside, gardening, craft activities and stick to a pre-bedtime routine. Sticking to a daily routine helps your brain prepare for sleep when the time comes.
Avoid vigorous exercises within four to six hours of bedtime. Regular exercise can be helpful for pain, and promotes good sleep, but vigorous exercise just before bedtime can be disruptive. Any vigorous or cardiovascular exercise should be completed at least six hours before bedtime. Relaxing exercises such as yoga can be done before bedtime in order to help initiate a restful night's sleep.
Patience is advised when beginning to follow healthy sleep hygiene guidelines. It may take some time to see the full effects of changing habits. Be kind to yourself!
Psychological Techniques
Psychological techniques that can help with sleep problems include cognitive behavioural therapy, relaxation training, meditation, and hypnosis. These techniques rely on a common set of skills:
- Deep muscle relaxation
- Focus elsewhere rather than on the pain
- Visual, sound, or other relaxing sensory imagery
- Distancing oneself from the persistent pain
Similar techniques are also used by people who want to manage stress and/or persistent pain during the day.
Cognitive Behavioural Therapy Eliminates Negative Thoughts
Cognitive behavioural therapy (CBT) for insomnia focuses on controlling or eliminating negative thoughts, worries, and behaviours, and replacing them with more positive thoughts and behaviours so the individual can fall asleep.
Sessions typically include several weekly visits with a therapist, but this therapy is also available online. Medical literature has shown CBT can be very effective in treating insomnia.
When coupled with the deep breathing technique that follows, these CBT techniques can be beneficial in improving sleep and decreasing the perception of pain by retraining the brain. Take a look at the Sleepio website for more useful information.
Deep Breathing Exercises Make Sleep Easier
There are a whole host of guided deep breathing techniques on YouTube that can help make sleep easier. Some audio sessions give you instructions at the beginning and leave you to listen to the sounds while practising the breathing techniques whereas others are more guided in their approach and you are ‘accompanied’ through your breathing ‘journey’. You may need to try out a few different sessions to find out what works best for you. You can use a SMART system like voice activated Alexa, or Siri to turn on the session without you needing to touch it and you are also able to set the session to end automatically.
While preparing for any persistent pain coping method, it is important to learn how to use focus and deep breathing techniques to relax the body. Learning to relax takes practice, especially while in pain. It is beneficial to be able to release muscle tension throughout the body and start to remove attention from the pain.
Coping techniques for persistent pain begin with controlled deep breathing, as follows:
- Set yourself in a relaxed, reclined position in a dark room and either close both eyes or focus on a point.
- Slow down your breathing and take deep breaths, using the chest (and not the abdomen). If distracted, thinking of a word, such as "relax" to help control your breathing and gain focus can be helpful. This process may be performed by repeating the syllable "re" while breathing in and "lax" while breathing out.
- Continue with about 2 to 3 minutes of controlled breathing.
After relaxation and focus are achieved, imagery techniques can be used.
Ten specific imagery and persistent pain control techniques that are effective for pain management include:
- Altered focus. This is a favourite technique for demonstrating how powerfully the mind can alter sensations in the body. Altered focus includes focusing attention on a specific non-painful part of the body and altering sensation in that part of the body. For example, imagining the belly. This process takes the mind away from focusing on the source of pain in another area of the body.
- Dissociation. As the name implies, this persistent pain technique involves mentally separating the painful body part from the rest of the body, or imagining the body and mind as separate, with the persistent pain distant from one’s mind. For example, imagine the painful lower back sitting on a chair across the room and telling it to stay sitting there, far away from the mind.
- Sensory splitting. This technique involves dividing the painful sensation (pain, burning, pins and needles) into separate parts. For example, if the pain feels hot, the sensation of the heat is focused upon (and not on the hurting).
- Mental anaesthesia. This method involves imagining an injection of numbing anaesthetic into the painful area. Similarly, imagining a soothing and cooling ice pack being placed onto the painful area can help reduce the perception of pain.
- Mental analgesia. Building on the mental anaesthesia concept, this technique involves imagining an injection of a strong pain-relieving agent, into the painful area. An alternative method is imagining the brain producing a massive amount of endorphins, the natural pain-relieving substance of the body, and having it flow to the painful areas.
- Age progression/regression. Using the mind’s eye to project oneself forward or backward in time to a pain-free state or experiencing much less pain. Then instructing yourself to act "as if" this image were true.
- Symbolic imagery. Envisioning a symbol that represents persistent pain, such as a loud, irritating noise or a painfully bright light bulb. Gradually reducing the irritating qualities of this symbol, for example dimming the light or reducing the volume of the noise, thereby reducing the pain.
- Positive imagery. Focusing your attention on a pleasant place, such as the beach, or the mountains, etc. - where a carefree, safe, and relaxed state may be achieved.
- Counting. Silent counting is a good way to deal with painful episodes. Counting may include the number of breaths, holes in an acoustic ceiling, floor tiles, or simply conjuring up mental images and counting them.
- Pain movement. Moving persistent pain from one area of your body to another, where the pain is easier to cope with.
Some of these techniques are probably best learned with the help of a professional, and it usually takes practice for these methods to become effective in helping alleviate persistent pain. It is often advisable to work on pain coping strategies for about 30 minutes 3 times a week. With practice, relaxation and persistent pain control can become strong and last for a long time.
After learning these techniques, persistent pain relief and relaxation can be produced with just a few deep breaths. These techniques can then be used while being engaged in any activity, working, talking, etc. With enough experience, a greater sense of control over the persistent pain and its effects on life can be felt.
Sleep Apnoea
A number of beneficiaries report suffering from sleep apnoea. This is when your breathing stops and starts while you sleep. The most common type is called obstructive sleep apnoea (OSA).
Symptoms of sleep apnoea mainly happen while you sleep. They include:
- breathing stopping and starting – pauses in breathing might be something your partner notices
- making gasping, snorting or choking noises
- waking up a lot
- loud snoring
During the day, it is likely that you will feel the effects of this such as feeling very tired, finding it hard to concentrate, having a headache or suffering from mood swings.
It is a good idea to contact your GP if you think you might have sleep apnoea. You might be waking with a start, or if you share a bed with someone they might have noticed you gasping for breath. Sleep apnoea can be serious if it's not diagnosed and treated. If a GP thinks you might have sleep apnoea, they may refer you to a specialist sleep clinic for tests. You may be given devices to wear that will monitor your breathing and heartbeat while you sleep so an accurate picture can be assessed of what is going on while you sleep.
Sleep apnoea does not always need to be treated if it's mild. However many people need to use a device called a CPAP machine. You'll be given this for free on the NHS if you need it.
CPAP machine
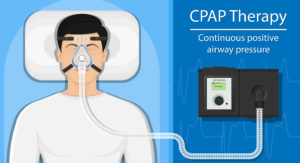 A CPAP machine gently pumps air into a mask you wear over your mouth or nose while you sleep. A CPAP machine can help:
A CPAP machine gently pumps air into a mask you wear over your mouth or nose while you sleep. A CPAP machine can help:
- improve your breathing while you sleep by stopping your airways getting too narrow
- improve the quality of your sleep and help you feel less tired
Using a CPAP machine may feel strange or awkward at first, but try to keep using it. It works best if you use it every night but reports are that it can take up to 6 months to get used to it.
Things you can do to help with sleep apnoea
If you have been diagnosed with sleep apnoea, there are some things you can do to help. These may be all you need to do if your sleep apnoea is mild.
- If you're overweight trying to lose weight can help.
- Sleep on your side, you can buy a special pillow or bed wedge to help keep you on your side.
- Do not smoke.
- Avoid drinking too much alcohol – especially shortly before going to sleep.
- Do not take sleeping pills unless recommended by a doctor – they can make sleep apnoea worse.
Sleep apnoea happens if your airways become too narrow while you sleep. This stops you breathing properly.
Sleep apnoea has been linked to:
- obesity;
- having a large neck;
- getting older – although children and young adults can also get it;
- having other family members with sleep apnoea;
- smoking and drinking alcohol;
- having large tonsils or adenoids;
- sleeping on your back.
Contact us for help and further information
We’ve talked above about some of the causes of a less than restful night’s sleep, but this is by no means an exhaustive list. If you are having issues sleeping please call and speak to the Health & Wellbeing team on 01480 474074.
We’ll try to unpick what is going on and may suggest a chat with one of our medical advisors, or your own GP. This combined with some tried and tested advice could help you begin to enjoy a better night’s sleep more often.